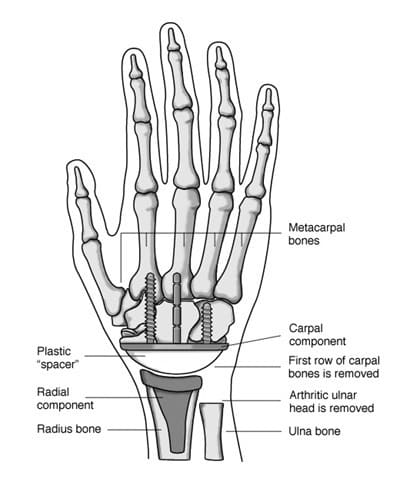
Description
The bursa is a slippery sac between the loose skin and the bones of your elbow. The bursa allows the skin to move freely over the underlying bone. It is located at the tip of the elbow. Normally, the bursa is flat and it’s hard to tell it is even there. If the bursa becomes irritated or inflamed, a condition known as elbow bursitis develops.
Risk Factors/Prevention
Common causes of elbow bursitis include:
- Trauma: A hard blow to the tip of the elbow could cause the bursa to produce excess fluid and swell.
- Prolonged pressure: Leaning on the tip of the elbow for long periods of time on hard surfaces such as a tabletop may cause the bursa to swell. Typically, this type of bursitis would develop over several months.
- Infection: If the tip of the elbow has an injury that breaks the skin, such as an insect bite or a scrape, bacteria may get inside the bursa and cause an infection. The infected bursa produces fluid, redness and swelling. If the infection goes untreated, the fluid may turn to pus.
- Medical conditions: Certain conditions such as rheumatoid arthritis and gout are associated with development of elbow bursitis.
Symptoms
Swelling is often the first symptom. The skin on the back of the elbow is loose, so you may not notice small amounts of swelling right away. As the swelling continues, the bursa gets larger. This causes pain as the bursa is stretched, since the bursa contains nerve endings. The swelling may get large enough to restrict motion in the elbow.
If the bursitis is infected, the skin becomes red and warm. If the infection is not treated right away, it may spread to other parts of the arm or move into the bloodstream. This can cause serious illness.
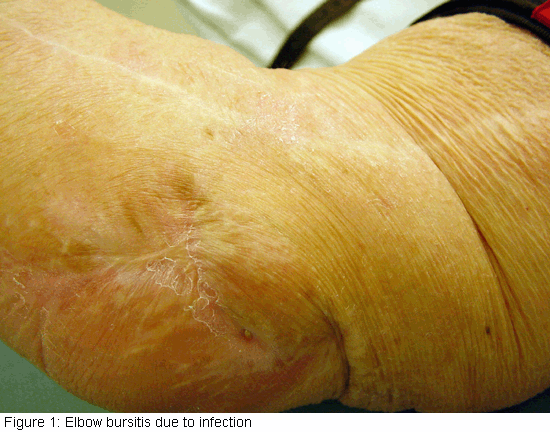
See your doctor to diagnose elbow bursitis. You may need an X-ray so the doctor can look for a foreign body or a bone spur. Bone spurs are often found on the tip of the bone in the elbow in patients who have recurrent problems with elbow bursitis.
Treatment Options: Nonsurgical
First, the doctor must determine whether the bursitis is due to an infection. If the doctor suspects this, fluid removal (aspiration) of the swollen area may be recommended. This is commonly performed as an office procedure. Fluid removal helps relieve symptoms and gives the doctor a sample that can be looked at in a laboratory to identify if any bacteria are growing.
This also lets the doctor know if a specific antibiotic is needed to fight the infection.
Often, the doctor may start you on antibiotics before the exact bacteria can be identified. This is done to prevent the infection from progressing. The antibiotic that the doctor recommends in this case will cover a number of possible infections.
If the bursitis is not from an infection, it is treated with elevation, ice and other nonoperative treatments such as an elbow pad and avoidance of direct pressure on the swollen elbow. Oral medications such as ibuprofen or other anti-inflammatories may also be used.
If the swelling and pain do not respond to these measures, your doctor may recommend removing fluid from the bursa and injecting a corticosteroid medication into the bursa. The steroid medication is an anti-inflammatory that is stronger than the medication that can be taken by mouth.
Treatment Options: Surgical
Infected bursa that do not improve with antibiotics and/or removing fluid from the elbow may require surgery. Patients who have surgery for elbow bursitis may need to stay in the hospital for a period of time.
If elbow bursitis is not a result of infection, surgery may be needed if nonoperative treatments don’t work. Surgery to remove the bursa is usually performed as an outpatient procedure. The surgery does not disturb any muscle, ligament or joint structure. Physical therapy after surgery is not always needed. Postoperative casting or prolonged immobilization is not typically required.

 Diagnosis and treatment
Diagnosis and treatment