Description
Carpal tunnel syndrome is a common source of hand numbness and pain. It is more common in women than men and affects up to 10 percent of the population. It is caused by increased pressure on a nerve entering the hand through the confined space of the carpal tunnel.
The median nerve travels from the forearm into your hand through a tunnel in your wrist. The bottom and sides of this tunnel are formed by wrist bones and the top of the tunnel is covered by a strong band of connective tissue called a ligament.
Your doctor may make the diagnosis by discussing your symptoms and examining you. If symptoms continue to bother you, electrical testing of the nerve function is often performed to help confirm the diagnosis and clarify the best treatment option in your case.
Symptoms
Symptoms usually begin gradually without a specific injury. Numbness, tingling and pain in the hand are common. You may experience an electric-like shocking feeling. The thumb side of the hand is usually most involved. Symptoms at night are common and may awaken you from sleep.
During the day symptoms frequently occur with holding a phone, reading or driving. Symptoms may occur at any time. Moving or shaking the hands often helps decrease symptoms. Sometimes strange feelings and pain will travel up the arm.
Initially symptoms come and go, but over time they may become constant. A feeling of clumsiness or weakness can make delicate motions like buttoning buttons difficult and may cause you to drop things. If the condition is very severe, muscles in the palm may become visibly wasted.
Risk Factors
The actual cause is unknown in most people. Carpal tunnel syndrome is more common in women. In women, the swelling that occurs during pregnancy may cause symptoms, but those will frequently go away after delivery. Carpal tunnel syndrome becomes more common as we grow older and seems to affect people with certain medical conditions such as diabetes, thyroid conditions and rheumatoid arthritis more frequently.
Treatment Options
Symptoms can often be relieved without surgery. Treatment often begins with a brace or splint worn at night to keep the wrist in a natural position. Splints can also be worn during activities that aggravate symptoms. Simple medications such as Tylenol® or Advil® can help decrease pain. Changing patterns of hand use to avoid aggravating positions and activities may be helpful. A corticosteroid injection will often provide temporary relief, but symptoms may come back.
If your carpal tunnel syndrome continues to bother you and you do not gain relief from non-surgical treatments, surgery can be effective in diminishing symptoms. Because carpal tunnel syndrome is not a dangerous problem, the decision whether to have surgery is based mostly on the severity of your symptoms.
- If your symptoms are severe and won’t go away you may want to consider surgery.
- In more severe cases, surgery is considered sooner because other treatment options are less helpful.
- In very severe cases, surgery may be recommended to prevent irreversible damage.
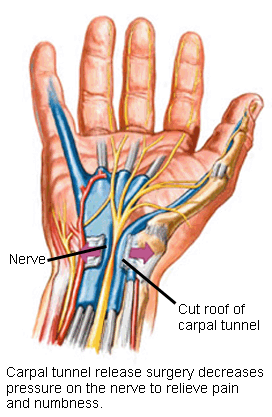 Treatment Options: Surgical
Treatment Options: Surgical
The strong roof of the carpal tunnel is cut during carpal tunnel surgery to increase the size of the tunnel and decrease pressure on the nerve. This is done through an incision in the palm or wrist. A small camera may be used to allow the surgery to be performed through a smaller incision.
Risks of the surgery include bleeding, infection and nerve injury. Some pain, swelling and stiffness are expected, but severe problems are rare.
After surgery, elevating the hand and moving the fingers helps minimize swelling and stiffness. Minor soreness in the palm is common for several months after surgery. Most patients have improvement following surgery, but recovery may be gradual.
When carpal tunnel syndrome has been present longer and the nerve is more severely affected, recovery is slower and less complete.

 The ceiling is the transverse carpal ligament. The median nerve runs from the forearm to the hand and directly through the carpal tunnel. This nerve controls some of your hand muscles and also allows sensation of your thumb, index, middle, and half of your ring finger. When this nerve is pressed and squeezed, carpal tunnel syndrome develops.
The ceiling is the transverse carpal ligament. The median nerve runs from the forearm to the hand and directly through the carpal tunnel. This nerve controls some of your hand muscles and also allows sensation of your thumb, index, middle, and half of your ring finger. When this nerve is pressed and squeezed, carpal tunnel syndrome develops.