Patients may have hip impingement for years before diagnosis because it’s rarely painful in its early stages. Early diagnosis is important; however, hip impingement if left untreated, can cause cartilage damage and osteoarthritis.
Once hip impingement becomes more advanced, symptoms include:
- General stiffness in the groin or front of the thigh.
- Running, jumping or sitting after flexing will also cause pain the groin region
What is hip impingement?
Hip impingement (femoro acetabular acetabular impingement) is a more recently recognized cause of hip pain in the active adult.
Hip impingement is caused by a lack of room or clearance between the neck of the femur and the rim of the socket (acetabulum). In a normal hip, there is a gliding motion of the round femoral head within the socket, but with an impinged hip, the gliding motion is disturbed. Dr. Downer states, “Mechanical problems do not always require surgical treatment; when symptoms affect function and lifestyle then surgery is justified.”
Dr. Downer, provides specialized care in hip restoration and replacement, and has a special interest in hip impingement conditions. Treatment options may include:
- First approach – Trying to control the pain with anti-inflammatory medications – If pain persists, surgical treatment may be necessary.
- Surgical treatment of hip impingement involves removing or correcting the cause of the reduced clearance between the neck of the femur and the rim of the socket (acetabulum). This may require arthroscopic surgery of the hip to remove diseased portions of the acetabulem (labrum) as well as femoral neck.
- In severe cases, it may be necessary to correct the deformity and reshape the femoral neck and/or rim of the socket through a larger incision. In cases of malposition of the socket, a redirecting procedure, called a periacetabular osteotomy (PAO) may be required.
Don’t let a hip impingement slow down your healthy, active lifestyle. Find out treatment options so that you can continue doing the things you love. Call Orthopedic Specialists of Seattle and schedule a consultation with Dr. Downer at (206) 633-8100.

 Treatment Options: Surgical
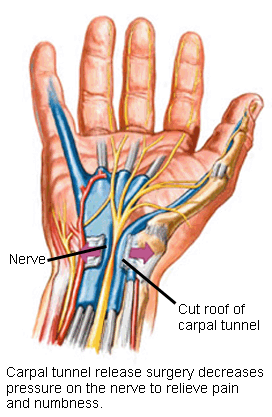
Treatment Options: Surgical The ceiling is the transverse carpal ligament. The median nerve runs from the forearm to the hand and directly through the carpal tunnel. This nerve controls some of your hand muscles and also allows sensation of your thumb, index, middle, and half of your ring finger. When this nerve is pressed and squeezed, carpal tunnel syndrome develops.
The ceiling is the transverse carpal ligament. The median nerve runs from the forearm to the hand and directly through the carpal tunnel. This nerve controls some of your hand muscles and also allows sensation of your thumb, index, middle, and half of your ring finger. When this nerve is pressed and squeezed, carpal tunnel syndrome develops.