Osteochondral Lesions
Osteochondral lesions are injuries to the talus (the bottom bone of the ankle joint) that involve both the bone and the overlying cartilage. They may also be called osteochondritis dessicans or osteochondral fractures. These injuries may include softening of the cartilage layers, cyst-like lesions within the bone below the cartilage, or fracture of the cartilage and bone layers. Throughout this article, these injuries will be referred to as osteochondral lesions of the talus (OLT).
Anatomy
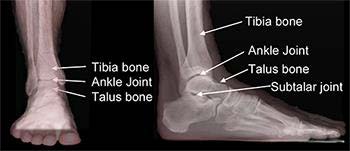
The talus is the bottom bone of the ankle joint. Much of this bone is covered with cartilage. The tibia and fibula bones sit above and to the sides of the talus, forming the ankle joint. This joint permits much of the up (dorsiflexion) and down (plantarflexion) motion of the foot and ankle. The blood supply to the talus is not as rich as many other bones in the body, and as a result, injuries to the talus sometimes are more difficult to heal than similar injuries in other bones.
Symptoms
OLTs usually occur after an injury to the ankle, either a single traumatic injury or as a result of repeated trauma. Common symptoms include prolonged pain, swelling, catching, and/or instability of the ankle joint. Symptoms can be vague. After an injury such as an ankle sprain, the initial pain and swelling should decrease with appropriate attention (rest, elevation). Persistent pain in spite of appropriate treatment after several months may raise concern for an OLT.
You may feel pain primarily at the lateral (outside) or medial (inside) point of the ankle joint. Severe locking or catching symptoms, where the ankle freezes up and will not bend, may indicate that there is a large osteochondral lesion or even a loose piece of cartilage or free bone within the joint.
Causes
The majority of OLTs, as many as 85%, occur after a traumatic injury to the ankle joint. Ankle sprains are a common cause of OLTs. With this type of injury, a section of the talus surface may impact another part of the ankle joint (tibia or fibula) and injure the talus. Some patients, however, have no history of an injury to their ankle.
Diagnosis
Foot and ankle orthopedic surgeons diagnose OLTs with a combination of clinical and special studies. Your surgeon may have a suspicion that you have this type of injury from the history you provide and their physical examination. Imaging is necessary to confirm the diagnosis. Occasionally, regular X-rays can show an OLT but frequently additional imaging is needed, such as a CT scan or an MRI.
Treatments
Once the diagnosis has been confirmed, treatment may be surgical or non-surgical, depending on the nature of the OLT, presence of other injuries, and patient characteristics.
Non-surgical Treatment
Non-surgical treatment is appropriate for certain lesions and usually involves immobilization and restricted weightbearing. This may be followed with gradual progression of weightbearing and physical therapy. The goal of non-surgical treatment is to allow the injured cartilage and bone to heal. Patients may have an OLT that is present and doesn’t cause pain or limitations or a lesion that becomes painful but improves. In these cases, no additional treatment is necessary. It was once believed that all OLTs progress and worsen with time. This has been shown to no longer be true.
Surgical Treatment
Other lesions may be more appropriately treated with surgery. The goals of surgery are to restore the normal shape and gliding surface of the talus in order to re-establish normal mechanics and joint forces. The hope is to minimize symptoms and limit the risk of developing arthritis.
Depending on the characteristics and location of the OLT, surgery may done arthroscopically or by opening the skin. Arthroscopy uses a camera and small instruments to view and work within the joint through small incisions. It may not be possible to properly treat certain lesions arthroscopically due to the size or location of the lesion. Treatments may include debridement (removing injured cartilage and bone), fixation of the injured fragment, microfracture or drilling of the lesion, bone grafting the bone cyst below the cartilage, and/or transfer or grafting of bone and cartilage. You and your foot and ankle orthopedic surgeon can discuss these treatment options and decide which one is best. Often, there may be several treatment options.
If you have any underlying conditions that may predispose to an OLT such as ankle instability, ankle impingement, a high arched (cavovarus) foot, or tight calf muscles, it may be necessary to correct these problems at the time of surgery as well.
Recovery
Recovery after OLT treatment varies depending upon the nature of the lesion and the treatment. Most treatments require a period of immobilization and restricted weightbearing that can range from several weeks to several months. More involved procedures that include bone grafting or cartilage transfer may require a longer period of recovery.
The results of non-surgical treatment of OLTs have been disappointing. Most studies show that full resolution of the pain from an OLT occurs in less than half of cases. Studies examining the outcomes after surgical debridement and microfracture (drilling) of OLTs have shown that more than 70% of patients have a good or excellent outcome. Procedures that transfer bone or cartilage to an OLT also have good outcomes. In general, the best results can be expected for smaller lesions.
Risks and Complications
All surgeries come with possible complications, including the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications, such as infection or wound healing problems, are uncommon after arthroscopic ankle surgery. More complex procedures with an open surgical approach or bone or cartilage transfer may have additional risks. In addition to standard surgical risks, additional complications may include the failure of any transplanted tissue (bone or cartilage). Despite surgery going as well as possible, there is still a chance the pain will persist requiring additional treatment in the future.
