Talar Fracture
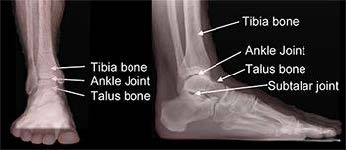
The talus bone makes up part of the ankle joint and the subtalar joint. The ankle joint allows for up-and-down motion and the subtalar joint supports side-to-side motion. A talar fracture is a break in the talus bone that often involves both of these important joints.
The ankle and foot must be well-aligned for proper function. The goal of surgery is to realign the bone pieces and restore the normal bone shape. The surgery also will restore the function of the ankle and subtalar joints. This surgery should reduce the chances of developing arthritis or losing blood supply to the bone.
Diagnosis
Talar fracture surgery is needed if the bone has shifted or broken through skin, if the nerves or blood vessels are damaged, or if there is an uneven cartilage surface in the ankle or subtalar joints.
Surgery should not be performed in fractures that haven’t shifted, patients who are sick or elderly and cannot risk having anesthesia, or in patients who have very injured or burned skin over the fracture.
Treatment
Talar surgery puts the talus bone back together as best as possible. During surgery you may have a general anesthetic and be completely asleep or have your leg numbed with a nerve block. The bone is exposed with one or two incisions and the broken pieces are realigned. When the fracture is in the appropriate position, your foot and ankle orthopedic surgeon will fix the bone pieces together with plates and/or screws. Then the incisions are closed and the foot is placed into a cast or splint.
Specific Techniques
Every break has a unique fracture pattern, so surgery requires its own tailored approach. Most surgeons will place a tourniquet on the leg above or below the knee. Your surgeon will then make one or two incisions over the bone on either side of the foot. There are important tendons, nerves and blood vessels that are carefully moved out of the way in order to expose the fractured bone.
Your surgeon uses many different tools to move the fractured bone into the appropriate position. The bone pieces are then held in position with temporary pins or clamps and the positioning is checked with an X-ray. When the positioning is correct, the surgeon will place permanent screws and plates across the fracture. The final position of the bone, joints and screws/plates is confirmed on X-ray. The wounds are closed with layers of suture before the foot is placed into a cast or splint below the knee.
Recovery
You may have a short stay in the hospital depending on the severity of the fracture and other injuries. Your surgeon will monitor the incisions and bone healing for the first several weeks after surgery. You should avoid putting weight on the leg until approved by your surgeon. If the fracture was sufficiently stabilized with the plates and screws, you may be placed into a removable boot that will allow you to start moving the ankle to combat stiffness and to bathe.
For certain fractures, your surgeon may decide to place a new cast. You typically will be on crutches, putting no weight on the injured foot for 8-12 weeks after surgery until X-rays show that the fracture has healed sufficiently.
You can expect to have some degree of pain and stiffness after treatment. Some patients will require physical therapy. The complete recovery may take six to 12 months from the time of injury.
Risks and Complications
All surgeries come with possible complications, including the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Immediate possible complications from talar surgery include wound healing problems, excess swelling, and infection. Patients typically receive intravenous antibiotics prior to surgery, but an infection still may develop in the days and weeks after surgery.
Most wounds will take about 2-4 weeks to heal safely, but this can take much longer if there were traumatic wounds, or if the patient has diabetes or smokes. In the hours to days after surgery, the foot may swell considerably after a talar fracture. If the swelling gets to be too much it may limit blood flow to the foot, resulting in a condition called compartment syndrome. There also is a chance that the bone cannot be put back to its original state, a complication called malunion. Any of these complications may require another procedure to correct.
Some of the most common long-term complications after talar fractures are arthritis and a condition called avascular necrosis (AVN) of the talus. Arthritis can occur after any severe injury to the ankle and is more likely if the fracture has shifted. AVN, which is the death of bone tissue due to a lack of blood supply, also is more frequent with fractures that have shifted.
FAQs
Will I develop arthritis after surgery?
Even if the bones heal well, the talus may develop arthritis at any of three joints: the ankle joint, the talonavicular joint, or the subtalar joint. The subtalar joint is directly below the ankle joint and is responsible for most of the side-to-side motion of our foot. Many patients experience some degree of pain, stiffness, and/or weakness after surgery.
What are the treatment options if I develop arthritis?
If arthritis develops in one or more joints after a talus fracture, it can be treated with medication, braces, injections, and activity modification. If these treatments are unsuccessful, your foot and ankle orthopedic surgeon may discuss additional surgery with you.
What if I develop avascular necrosis of the talus?
Avascular necrosis (AVN) of the talus can be a serious complication of fractures of the talus. AVN can occur with any injury depending on the severity of the fracture. If it does develop, it is not always painful. If it is painful then many of the same treatments for arthritis may be indicated, including fusion surgery.
Does smoking affect my outcome?
Yes. Smoking affects your body’s ability to heal the broken bone as well as the surrounding tissues. Smoking also increases the risk of infection. You should quit smoking immediately in order to minimize these risks.
